 by Hillary O’Boyle, MD
by Hillary O’Boyle, MD
In a household with two pediatricians, we can handle most things when our child gets sick. So, when our previously healthy 7-month-old came down with a fever and cold symptoms, we weren’t overly concerned. His appetite was decreased and his nights were very restless, but we figured it would pass within a few days.
After 4 days of unrelenting fever, we started to worry. He still wasn’t drinking much, and I noticed he was breathing very fast even while asleep. I counted his respirations—60, sometimes even 70 breaths per minute—which persisted even when his fever was down. My husband and I agreed that if these symptoms continued for a fifth straight day, we would take him to an urgent care. We thought he might need a chest X-ray or some labs.
On Day 5, he was still not improving, with continued fevers and very few wet diapers. At that point, we knew he needed further evaluation.
Our urgent care visit turned into an ambulance trip to the hospital
While my husband was at work, I took our son to a nearby urgent care that afternoon. They checked his vital signs when we arrived, including his oxygen saturation. My heart dropped when I saw the number on the pulse oximeter. It was too low.
Being in medicine, I knew immediately that they would send us to a hospital, and because he was needing oxygen, we would have to go by ambulance. Also, being a hospital pediatrician myself, I was almost certain he would need to be admitted to the hospital. This was NOT what I had expected. My son was about to become a patient at the same hospital where I work.
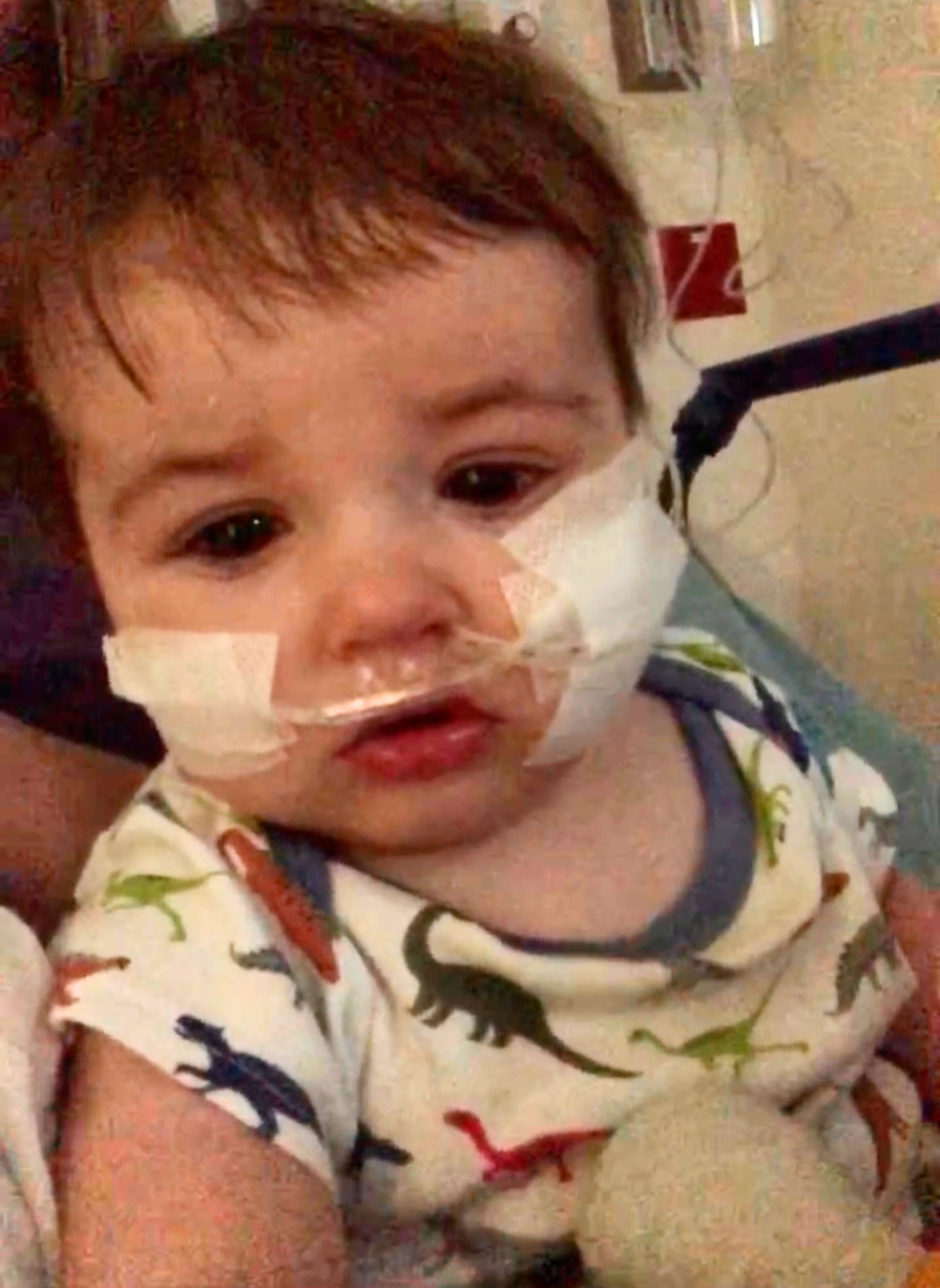
As I was laying on on the stretcher holding my sick little boy, it seemed like a bad dream. We were rolled into the ER and assigned to a room where, so many times, I had visited with sick patients as the doctor. It felt like a cruel role-reversal. Things happened quickly at first. He received Tylenol, a chest X-ray, and a swab to check for viruses. He was diagnosed with RSV, which wasn’t a surprise. The hospital was full of young children with RSV. I had cared for many of them in the days prior.
His X-ray was concerning for a concurrent bacterial pneumonia, so he was started on antibiotics. He also needed fluids due to dehydration, so the decision was made to place an IV. It was hard to watch, as I knew it would be, but I was not prepared for three unsuccessful attempts which left my son crying inconsolably and struggling to catch his breath. He was too dehydrated and his veins were too small. I was fortunate enough to know that there was another way for him to receive fluids, so I advocated for the placement of a nasogastric tube. This allowed him to receive fluids into his stomach through a tube in his nose, which turned out to be a much better and less traumatic option.
As this was all happening, they tried multiple times to remove the oxygen, however his saturations were still dropping. This was confirmation that he would indeed need to be admitted to the hospital.
Having not prepared for this when we left for urgent care, I found myself with no food or change of clothes, but I was grateful that my son was safe and getting the care he needed. My husband brought essential items and spent some time with us. We decided it was best for him to go home overnight, so at least one of us could get decent rest.
One of the most difficult nights I have ever experienced
Knowing the hospital was full, I’d expected we’d have to wait on some discharges before we would get a room (potentially several hours). Unfortunately, because there was a large queue in front of us, we stayed in the ER room for over 24 hours. Boarding in the ER was very challenging. The nursing staff was stretched so thin, and because we were already “admitted,” we were considered less urgent. We got fewer nursing assessments and check ins, but I know the nurses were doing their best.
My son and I were stuck sharing a single stretcher all night, and it was impossible for me to sleep. My son was only comfortable sleeping on my chest. He would scream and fight when anyone came in to check vitals or give meds, due to trauma from the unsuccessful IV sticks. If I needed to leave the room to get food or use the bathroom, someone had to come chaperone my son. It often took a while to find someone to do that. I felt helpless, scared, and lonely.
Fortunately, my son was able to be weaned off the oxygen the next morning. We waited all day in hopes that his fluid intake would improve. It finally did. His fever broke and we were ultimately discharged the next evening, directly from the ER room. We never got a hospital bed, even after more than 24 hours. I know many families endure a lengthier hospitalization, so overall I felt lucky that was not the case for us.
As a doctor, the experience of my son’s hospitalization for RSV has changed the way I practice medicine. I know firsthand the helplessness and vulnerability that a parent feels when their child is seriously ill and traumatized from medical intervention. I still feel that ache in my chest when I encounter a worried family who is desperate to comfort their sick child. I hope that one day there will be a vaccine for RSV so we can reduce the number of families that go through a similar—or worse—experience.
Hillary O’Boyle, MD, is a pediatrician at the Children’s Hospital of Richmond. Her story, like all others on this blog, was a voluntary submission. If you want to help make a difference, submit your own post by emailing Noah at [email protected]. We depend on real people like you sharing experience to protect others from misinformation.



